What if your practice’s financial health were in the hands of your billing process? Running a small internal medicine practice today means juggling more than just patient care; it’s about mastering medical billing and revenue cycle management. With shrinking reimbursements and an ever-evolving payer landscape, what was once simple now requires constant vigilance. For many providers, billing is no longer just a task; it’s a daily battle that can make or break your practice. Denied claims, missed opportunities, and delayed payments don’t just disrupt your day; they threaten the long-term success of your business. How can you stay ahead in this financial race? Let’s find out.
The Importance of Internal Medicine Billing in Small Practices
Internal medicine billing is more than a routine task; it’s a critical part of how services are translated into reimbursement. For small practices, this process includes:
- Coding encounters with CPT (Current Procedural Terminology) and ICD (International Classification of Diseases) codes.
- Submitting claims, managing denials, and following up on unpaid claims.
- Ensuring documentation supports the services billed.
Understanding how each of these components impacts financial health can help providers reduce revenue leakage. Efficient billing is essential to maintain healthy cash flow and the overall viability of small practices, especially when resources are limited.
Why Internal Medicine Billing Is Especially Challenging
Internal medicine is a complex specialty with a range of services that require specific billing expertise:
- Preventive care and wellness visits.
- Chronic disease management.
- Office-based E/M services.
- Post-discharge care.
These services each have their own coding rules, documentation requirements, and payer restrictions. For small practices, these complexities are often compounded by staffing shortages and limited resources, making accurate billing a continual challenge.
Top Revenue Challenges Faced by Small Internal Medicine Practices
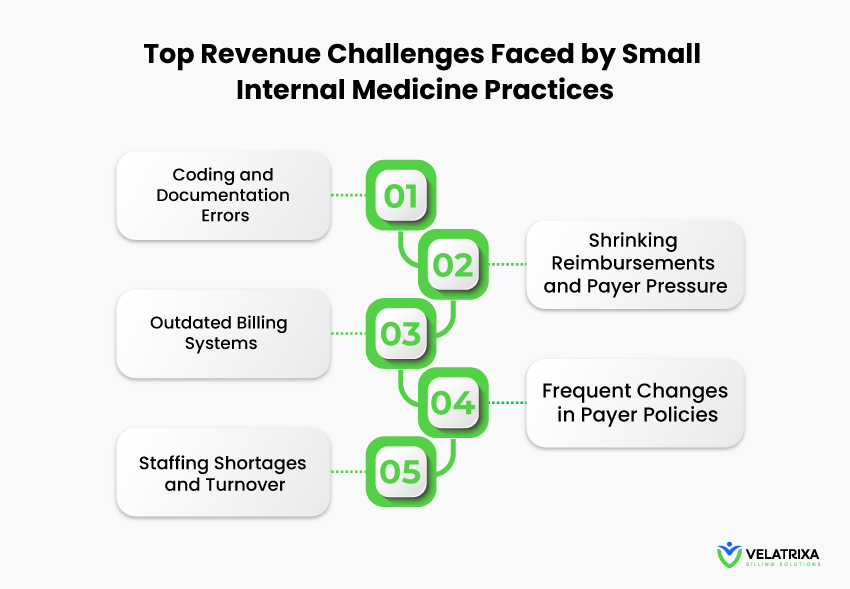
Medical billing may seem straightforward, but many internal medicine practices face a range of challenges that disrupt financial stability. Addressing these issues proactively is key to sustaining a practice. Here’s a breakdown of the most pressing challenges:
1. Coding and Documentation Errors
Errors in coding or incomplete documentation can lead to denied claims and underpayments, which may require a time-consuming process to resolve. Many small practices struggle to meet the documentation requirements for Evaluation & Management (E/M) services, leading to costly audits and claims that do not reflect the actual services provided.
2. Outdated Billing Systems
Despite technological advances, many small practices continue to rely on legacy billing systems that are not automated and lack real-time error checks. This causes manual errors, delays in claim submissions, and ultimately reduces revenue.
3. Staffing Shortages and Turnover
Staff turnover is a persistent issue in small practices. With high turnover rates for coders and billing personnel, practices face frequent backlogs and delays in claim submissions. Without experienced personnel, managing a complex revenue cycle becomes even harder, leading to denied claims and reduced revenue.
4. Shrinking Reimbursements and Payer Pressure
Insurance reimbursements continue to shrink, particularly from Medicare and commercial payers. Practices are expected to capture every penny they are owed, making it critical to manage claims accurately. Underpaid claims or missed opportunities for reimbursement can result in significant revenue loss.
5. Frequent Changes in Payer Policies
As payers frequently update their coverage criteria, modifiers, and documentation requirements, keeping up with these changes can be overwhelming. Small practices often lack the resources to ensure that they are compliant with the latest payer policies, which can lead to compliance risks and delayed payments.
Essential Coding Services for Internal Medicine Practices
Medical coding is the backbone of internal medicine billing, and it can significantly impact reimbursement rates and overall practice revenue. Accurate CPT (Current Procedural Terminology) and ICD (International Classification of Diseases) codes are essential to ensure that the services provided are correctly documented and reimbursed.
Below, we’ve outlined some of the essential coding services that practices rely on:
- Evaluation and Management (E/M) Coding: E/M codes are the most commonly used in internal medicine to reflect the level of care provided to patients, including office visits and consultations.
- Chronic Care Management (CCM): Codes for chronic disease management, including time spent managing care outside of face-to-face consultations.
- Preventive Services: Codes for annual wellness visits, screenings, and vaccinations.
- Telehealth Coding: Specialized codes for telemedicine consultations and remote care services.
- Procedure Codes: Specific codes for diagnostic tests, minor procedures, and specialty services.
To avoid common billing errors, it’s essential to use the right codes for the right services. Below is a cheat code table for common issues in internal medicine coding that can help ensure smoother claims processing and fewer denials.
Internal Medicine Coding Cheat Codes
| Challenge | Solution | Cheat Code Tip |
| E/M Coding Confusion | Consistently apply MDM (Medical Decision Making) or Time-based criteria based on visit complexity. | Use Time-based coding for straightforward cases, but switch to MDM-based coding for complex diagnoses or consultations. |
| Chronic Care Management Underbilling | Ensure that non-face-to-face care time (e.g., phone calls, care coordination) is captured correctly. | Use CPT 99490 for at least 20 minutes of care management and CPT 99439 for remote patient monitoring services. |
| Preventive Service Documentation Gaps | Be thorough in documenting patient consent, services provided, and follow-up care. | Ensure you’re billing correctly for services like AWV (Annual Wellness Visits) using CPT 99385-99397 for preventive care. |
| Telehealth Billing Confusion | Update your codes based on payer requirements for telemedicine visits, including new CPT codes for audio-only services. | Verify telehealth policies and use CPT 99201-99215 for video consultations and G2012 for audio-only consultations. |
| Procedure Code Errors | Ensure accurate use of diagnostic test and minor procedure codes. | Double-check that CPT 99211-99215 are being used for office visits, and CPT 36415 for blood draws. Use specific codes for diagnostic imaging or minor surgical procedures to avoid denials. |
Key Takeaways:
- Stay updated with coding guidelines, especially for E/M services and chronic care management.
- Use time-based or MDM-based coding as appropriate to capture the level of care accurately.
- Properly document preventive care and telehealth visits to ensure proper reimbursement.
- Regularly review coding cheat codes and strategies to avoid common mistakes that lead to denied claims and lost revenue.
Practical Strategies for Overcoming Billing Challenges in Internal Medicine
To remain financially viable in 2026, small practices must adopt strategies that help mitigate common billing challenges. Here’s how practices can navigate these obstacles:
1. Partner with Experts Who Understand Internal Medicine
Billing in internal medicine isn’t the same as in other specialties. Practices should seek billing services with coders who understand the unique needs of internal medicine. These professionals will help ensure accurate coding, reduce claim denials, and improve cash flow.
2. Invest in Modern Billing Systems
Upgrading to automated billing systems can streamline claims processing, reduce errors, and speed up reimbursements. Automated systems integrate real-time eligibility checks and payer-specific rules to ensure claims are submitted quickly and correctly.
3. Streamline Documentation Workflows
Accurate and detailed documentation is critical, especially for Evaluation & Management (E/M) services. Streamlining documentation workflows helps ensure that claims are billed accurately, reducing the risk of denials. Comprehensive documentation also supports higher reimbursements for chronic care management and preventive services.
4. Ongoing Training for Billing Staff
Billing guidelines and payer policies are constantly evolving. Continuous training ensures that coding teams stay up to date with changes, which helps minimize billing errors and improve accuracy in claims submissions.
5. Track and Address Revenue Leakage
Identify patterns in denials, underpayments, and rejected claims. Data analysis can reveal recurring issues that, if corrected, can significantly improve revenue cycle management and help practices capture lost revenue.
The Impact of 2026 Billing Changes: What You Need to Know
The 2026 healthcare billing landscape will bring several significant changes that small practices need to be prepared for. Here are the updates you should be aware of:
1. Major CPT Code Set Changes
The AMA’s 2026 CPT code set will include 288 new codes, 84 deletions, and 46 revisions. These changes will affect digital health and remote patient monitoring services, along with new codes for procedural and technology-based services. Practices will need to update their billing software to accommodate these new codes and avoid denials.
2. Expanded Telehealth Billing Rules
Medicare’s updates for 2026 offer expanded billing options for telehealth services, but they also come with changes regarding which services and providers are eligible for reimbursement. Practices will need to carefully review Medicare’s telehealth billing guidelines to ensure compliance.
3. ICD-10-CM Updates
The ICD-10-CM code updates set to take effect on October 1, 2025, will introduce hundreds of new diagnosis codes. Practices will need to prepare for these updates to ensure accurate coding and prevent revenue loss from coding errors.
4. Medicare Payment Policy Changes
CMS (Centers for Medicare & Medicaid Services) has finalized several changes that will affect Medicare Part B payments in 2026. These changes may include the removal of frequency limits for certain inpatient and outpatient visits, as well as adjustments to how consultations and critical care services are reimbursed. Small practices must stay aligned with these updates to avoid underpayment.
Action Plan for Providers in 2026
To thrive in 2026, small practices should:
- Update technology and billing workflows with the latest CPT/ICD code sets.
- Train staff on new documentation and compliance requirements.
- Reevaluate telehealth and remote patient monitoring billing policies.
- Partner with specialized billing services like Velatrixa to enhance revenue cycle management.
- Monitor payer trends and denials to improve revenue capture.
How Velatrixa Supports Internal Medicine Practices
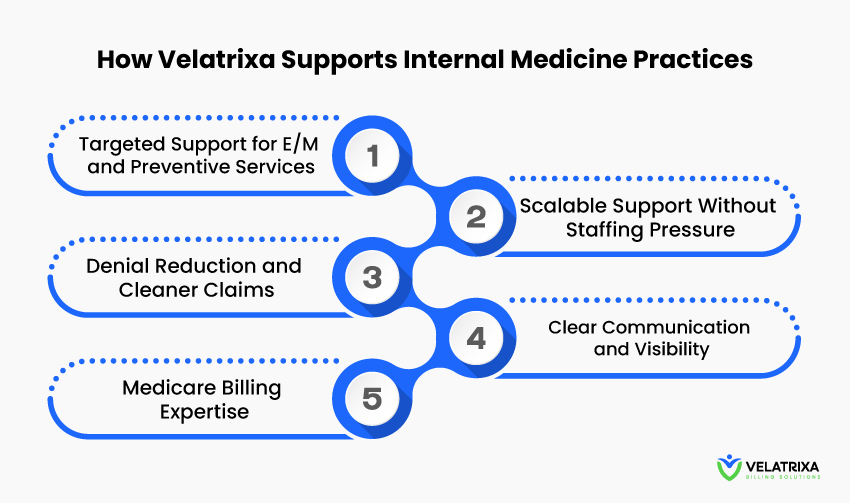
Velatrixa simplifies billing complexities, offering tailored support that includes:
Targeted Support for E/M and Preventive Services
We ensure accurate coding and documentation for Evaluation & Management and preventive services, so practices can maximize revenue without risking compliance.
Denial Reduction and Cleaner Claims
By addressing common denial triggers upfront, we help reduce claim rejections, leading to faster reimbursements and healthier cash flow.
Medicare Billing Expertise
We keep practices up-to-date with CMS rules, reducing the risk of errors and minimizing audit risk.
Scalable Support Without Staffing Pressure
Our billing support is available when you need it, without the need to hire, retrain, or invest in costly infrastructure.
Clear Communication and Visibility
With Velatrixa, practices can stay informed about billing trends, opportunities, and potential risks, all without drowning in reports or dashboards.
Conclusion:
As we approach 2026, it’s clear that medical billing will only grow more complex. Internal medicine practices are already navigating a difficult financial landscape, and the upcoming changes to CPT codes, ICD-10 updates, and Medicare billing policies will add new layers of complexity.
Small practices that stay informed and adapt quickly will be best positioned to thrive in the coming year. By leveraging modern billing systems, investing in staff training, and keeping up with payer policy changes, practices can reduce denials, capture lost revenue, and improve their overall financial health.
Ultimately, proactive billing management will be the key to ensuring long-term stability for small internal medicine practices in 2026 and beyond.
