In today’s complex healthcare landscape, ensuring that your acupuncture practice is properly credentialed and enrolled with insurance payers is essential for maintaining a steady revenue stream. Insurance credentialing for acupuncturists can be a detailed and time-consuming process, often leading to billing delays and claim denials if not handled correctly.
As more insurance companies begin covering acupuncture services for pain management, musculoskeletal disorders, and integrative treatments, providers must ensure they meet all payer credentialing requirements before submitting claims.
At Velatrixa, we understand the unique challenges acupuncture practices face with insurance enrollment, credentialing compliance, and acupuncture billing regulations. Our goal is to help acupuncture clinics streamline credentialing so practitioners can focus on delivering effective patient care while maintaining a healthy revenue cycle.
This guide explains the acupuncturist credentialing process step by step, common billing challenges, denial prevention strategies, and how professional acupuncturist credentialing services can accelerate approvals in 2026.
What Is Acupuncturist Credentialing and Why Does It Matters
Insurance credentialing is the process through which healthcare providers are verified and approved by insurance companies to provide medical services and receive reimbursement.
During the Acupuncturist credentialing process, insurance payers review a provider’s professional background, qualifications, and compliance status to determine whether they meet the insurer’s network participation standards.
Credentialing verification typically includes confirmation of:
- State acupuncture license
- Education and accredited acupuncture training
- National board certification (NCCAOM)
- Clinical experience and work history
- Malpractice insurance coverage
- National Provider Identifier (NPI)
- Compliance and exclusion checks
- Professional references
Insurance companies rely on credentialing to ensure that providers meet quality care and patient safety standards before allowing them to treat insured patients.
Acupuncturist Credentialing verification commonly includes background checks through databases such as:
- National Practitioner Data Bank (NPDB)
- Office of Inspector General (OIG) exclusion list
- National Plan and Provider Enumeration System (NPPES)
For acupuncture providers, credentialing is especially important as insurance coverage for integrative medicine and alternative therapies continues expanding.
Common insurance-covered acupuncture services include:
- Chronic pain management
- Back and neck pain treatment
- Migraine and headache therapy
- Post-surgical pain support
- Stress and anxiety management
- Musculoskeletal therapy
- Fertility support treatments
Without proper credentialing, acupuncturists may be unable to bill insurance payers or receive reimbursement for services provided.
Why Credentialing Is Critical for Acupuncture Practices
Credentialing plays a vital role in both financial stability and regulatory compliance for acupuncture clinics.
A properly credentialed acupuncture practice can:
- Participate in insurance networks
- Submit clean claims without eligibility rejections
- Expand access to insured patients
- Maintain compliance with healthcare regulations
- Increase patient trust and credibility
However, when credentialing is incomplete or inaccurate, acupuncture practices may experience:
- Claim denials due to provider ineligibility
- Delayed reimbursements
- Reduced patient access to insurance coverage
- Compliance risks
- Revenue cycle disruptions
As insurance coverage for acupuncture continues growing in 2026, credentialing accuracy will become even more critical for maintaining consistent reimbursement.
Challenges Faced by Acupuncturists in Insurance Credentialing
While credentialing is essential, the process can be complex and time-consuming for acupuncture clinics.
Many acupuncture providers encounter several common challenges.
Lengthy Credentialing Timelines
Insurance credentialing approvals can take 60 to 120 days, depending on the payer and application accuracy. These delays can significantly impact revenue, particularly for new acupuncture providers joining a clinic.
Typical credentialing timelines include:
| Credentialing Step | Average Time |
|---|---|
| CAQH profile setup | 1–3 days |
| Medicare enrollment | 45–60 days |
| Medicaid enrollment | 30–90 days |
| Commercial payer credentialing | 60–120 days |
| Final contract approval | 30–60 days |
If credentialing is not started early, practices may face months of unpaid services or limited patient access.
Limited Insurance Coverage for Acupuncture
Unlike many traditional medical specialties, acupuncture insurance coverage varies widely across states and payers.
Some insurers may require:
- Specific documentation for medical necessity
- Referrals from primary care physicians
- Approved acupuncture CPT codes
Understanding these payer-specific requirements is essential for avoiding billing issues.
Credentialing Errors and Application Rejections
Small documentation inconsistencies can cause significant delays.
Common credentialing mistakes include:
- Incomplete CAQH profiles
- Expired acupuncture licenses
- Missing NPI documentation
- Incorrect provider taxonomy codes
- Inconsistent provider information across applications
These issues can lead to rejected applications and extended approval timelines.
Re-Credentialing Requirements
Credentialing is not a one-time process.
Most insurance payers require providers to re-credential every two to three years.
Missing a re-credentialing deadline may result in:
- Temporary network termination
- Claim denials
- Loss of reimbursement eligibility
Maintaining an organized credentialing tracking system is critical for avoiding interruptions.
Step-by-Step Acupuncturist Credentialing Process
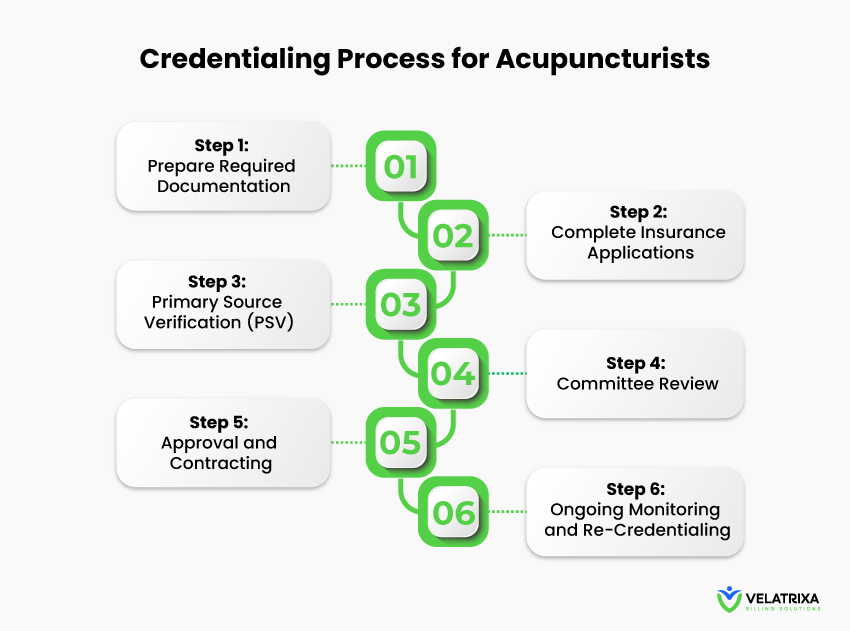
Credentialing for acupuncture providers involves several stages that must be completed accurately.
Below is a simplified breakdown of the process.
Step 1: Medicare and Medicaid Provider Enrollment
Government healthcare programs are often the first step in credentialing.
Medicare Enrollment
Medicare currently covers acupuncture for certain conditions, particularly chronic lower back pain.
Providers must enroll through the Medicare Provider Enrollment system and submit documentation including:
- CMS-855I provider enrollment form
- CMS-855R reassignment of benefits form
- NPI verification
- Practice ownership information
Once approved, providers receive a Medicare PTAN (Provider Transaction Access Number).
Medicaid Enrollment
Medicaid acupuncture coverage varies by state but typically requires:
- State acupuncture license verification
- NPI confirmation
- Compliance documentation
- Medicaid provider application
Completing Medicaid enrollment allows acupuncture providers to treat patients within state insurance programs.
Step 2: Commercial Insurance Credentialing
Commercial payer credentialing allows acupuncture providers to bill private insurance companies.
Applications are typically submitted to insurers such as:
- Aetna
- Cigna
- UnitedHealthcare
- Blue Cross Blue Shield
Required documentation usually includes:
- State acupuncture license
- NCCAOM certification
- DEA registration (if applicable)
- Malpractice insurance
- Updated curriculum vitae
- Clinic affiliation information
Once credentialing is approved, providers receive network participation contracts outlining reimbursement rates.
Step 3: CAQH Profile Setup and Management
The CAQH ProView system is widely used by insurance companies to streamline credentialing verification.
A properly maintained CAQH profile includes:
- Education and training history
- Professional work experience
- Licenses and certifications
- Malpractice coverage information
- Practice location details
Providers must re-attest their CAQH profile every 120 days to keep their information active.
Failure to maintain CAQH profiles is one of the most common causes of credentialing delays.
Step 4: Acupuncture Billing Setup and CPT Coding
Before submitting claims, acupuncture practices must establish compliant billing procedures.
Common acupuncture CPT codes include:
- 97810 – Initial acupuncture treatment without electrical stimulation
- 97811 – Additional acupuncture treatment sessions
- 97813 – Acupuncture with electrical stimulation
- 97814 – Additional sessions with electrical stimulation
Accurate coding and documentation are critical for avoiding insurance claim denials.
Step 5: Provider Network Enrollment and Contracting
After credentialing verification is complete, providers finalize payer contracts.
These agreements define:
- Reimbursement rates
- Covered acupuncture services
- Billing requirements
- Network participation terms
Understanding these contract terms helps acupuncture practices maximize reimbursement and prevent billing issues.
Acupuncturist Credentialing Application Checklist
Preparing credentialing documents in advance can significantly accelerate approvals.
Essential Acupuncture credentialing documents include:
Provider Identity Information
- Full legal name
- Date of birth
- Government identification
- Social Security number (for enrollment)
Provider Identification
- National Provider Identifier (NPI)
- NPI confirmation from NPPES
Professional Licensing
- Active state acupuncture license
- License verification documentation
- License expiration dates
Education and Training
- Acupuncture school diploma
- Certification documentation
- Training completion dates
Board Certification
- NCCAOM certification status
- Certification renewal documentation
Professional Work History
- Updated curriculum vitae
- Previous practice affiliations
Malpractice Insurance
- Current malpractice policy
- Coverage limits
- Claims history
Compliance Verification
- NPDB self-query
- OIG exclusion check
- HIPAA compliance documentation
Having these documents prepared can reduce credentialing approval timelines significantly.
Credentialing Timeline Overview
Acupuncturist credentialing timelines vary depending on the payer and documentation completeness.
Typical approval timelines include:
| Credentialing Step | Average Time |
|---|---|
| CAQH profile setup | 1–3 days |
| Medicare enrollment | 45–60 days |
| Medicaid enrollment | 30–90 days |
| Commercial payer credentialing | 60–120 days |
| Contract finalization | 30–60 days |
It is recommended that acupuncture providers begin credentialing at least 3-4 months before accepting insured patients.
The Insurance Enrollment Process for Acupuncturists
Once you are credentialed, you can start the insurance enrollment process, which is equally important for billing and reimbursement.
1. Verify Insurance Eligibility
Before providing services, always verify the insurance coverage of your patients. This step ensures that they are eligible for acupuncture treatments under their plan.
2. Submit Claims
After providing treatment, submit claims to the insurance company. Ensure that claims are accurate, using the correct CPT and ICD-10 codes for the services rendered. Claims can be submitted electronically or through paper forms, depending on the insurer’s preferences.
3. Track Claims and Follow-Up
It’s essential to track the status of your claims to ensure timely processing. Follow up on any denied or delayed claims promptly to avoid long payment cycles.
4. Reconcile Payments
Once payments are received, post them in your system and reconcile any discrepancies between what was billed and what was paid. Accurate reconciliation helps ensure that your practice maintains financial transparency.
5. Patient Billing
After insurance payments are applied, bill patients for any outstanding balance. Offer flexible payment options to maintain patient satisfaction.
Key Challenges in Acupuncture Credentialing and Billing
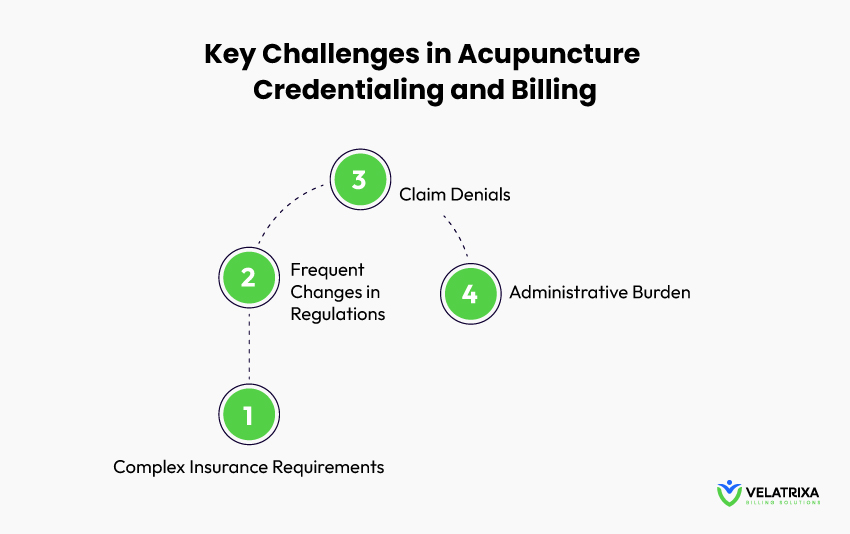
Acupuncturists face a variety of challenges when it comes to credentialing and billing, including:
1. Complex Insurance Requirements:
Each insurance provider has its own requirements for acupuncturist credentialing and billing. Managing these differences can be time-consuming and overwhelming.
2. Frequent Changes in Regulations:
Health insurance regulations, particularly Medicare credentialing requirements, change frequently, and staying updated on these changes is essential to avoid errors.
3. Claim Denials:
Incorrect coding, missing documentation, and administrative errors often lead to claim denials, delaying reimbursements.
4. Administrative Burden:
Handling credentialing and billing in-house requires significant time and effort, which could otherwise be spent on patient care and improving clinical practices.
The Benefits of Outsourcing Credentialing and Billing
Outsourcing credentialing and billing tasks to specialized providers like Velatrixa offers several key advantages:
- Expertise and Compliance: Outsourcing ensures that Acupuncturist credentialing and billing processes are handled by professionals who are up-to-date on industry regulations, ensuring compliance and reducing errors.
- Improved Efficiency: By outsourcing these tasks, you streamline your operations, leading to faster reimbursements and improved cash flow.
- Cost Savings: Outsourcing eliminates the need for additional in-house staff, saving overhead costs related to training, software, and administrative tasks.
- Focus on Patient Care: Outsourcing these processes frees up your time to focus on patient care, ensuring that you can deliver high-quality treatments without distraction.
Conclusion
Insurance credentialing is one of the most important administrative processes for acupuncture practices. Proper credentialing ensures providers can participate in insurance networks, receive reimbursement for treatments, and remain compliant with healthcare regulations. However, the credentialing process can be complex and time-consuming when managed internally.
By partnering with experienced acupuncturist credentialing professionals like Velatrixa, acupuncture practices can streamline provider enrollment, reduce claim denials, and ensure faster approvals across Medicare, Medicaid, and commercial insurance payers.
With expert credentialing support, acupuncturists can focus on delivering high-quality patient care while maintaining a stable and efficient revenue cycle.
