Behavioral health providers in 2026 are facing rising patient demand but tighter reimbursements, creating serious pressure on cash flow. Stricter payer rules, staffing shortages, and growing administrative workload are increasing the risk of revenue loss due to denials, authorization delays, and billing errors.
For psychiatrists, therapists, psychologists, ABA providers, and addiction treatment centers, Behavioral Health Revenue Cycle Management (RCM) is now essential for financial stability. With payers closely reviewing medical necessity, documentation, and telehealth compliance, even small billing mistakes can lead to delayed or lost payments. This is why more practices are relying on specialized behavioral health medical billing services to improve collections and reduce denials.
At Velatrixa, we help providers optimize their revenue cycle with accurate billing, proactive denial management, and end-to-end RCM solutions designed to maximize reimbursements.
What Is Behavioral Health Revenue Cycle Management?
Behavioral Health Revenue Cycle Management is the process of managing all financial and administrative tasks related to reimbursement for mental health and substance abuse treatment. The process begins when a patient schedules an appointment and continues until the provider receives full payment for services rendered.
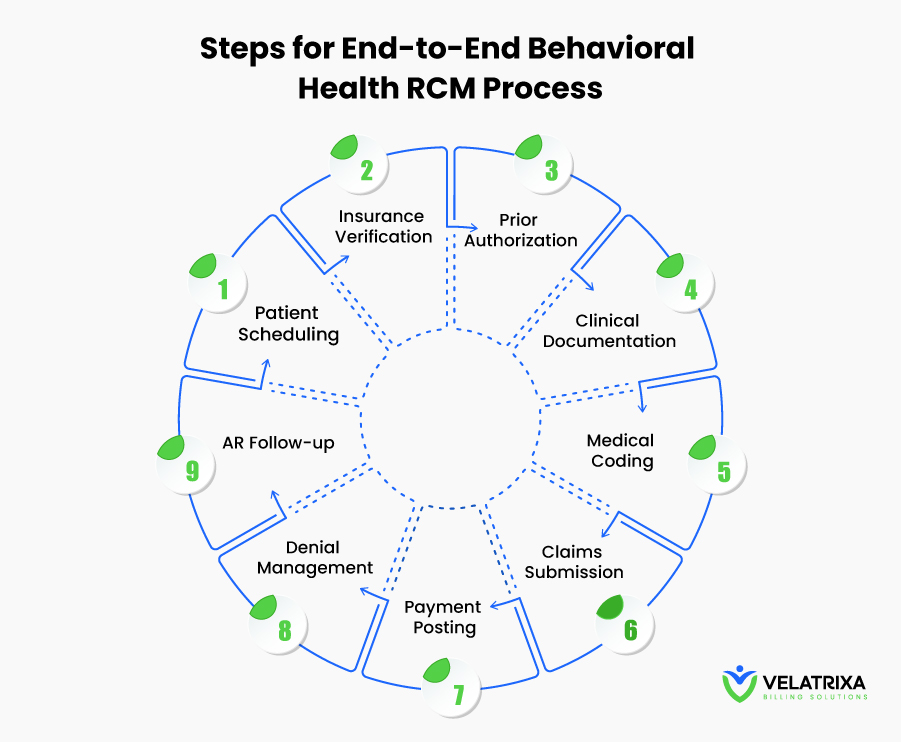
Behavioral health RCM includes:
- Insurance eligibility verification
- Prior authorization management
- Behavioral health medical coding
- Claims submission
- Denial management and appeals
- Payment posting
- Accounts receivable follow-up
- Patient billing and collections
A strong behavioral health revenue cycle management strategy helps providers improve cash flow, reduce claim denials, accelerate reimbursements, and maintain compliance with payer regulations.
Unlike traditional healthcare billing, behavioral health billing services require specialized expertise due to time-based CPT coding, medical necessity reviews, telehealth regulations, and payer-specific authorization requirements.
Without efficient behavioral health RCM processes, providers often struggle with delayed insurance payments, high denial rates, aging AR, and administrative burnout.
Why Behavioral Health Billing Has Become More Challenging
Behavioral health billing has become increasingly difficult because insurance companies now apply stricter reimbursement guidelines to mental health and substance abuse treatment claims.
One of the biggest challenges providers face is prior authorization management. Services such as ABA therapy, intensive outpatient programs (IOP), partial hospitalization programs (PHP), and substance abuse treatment frequently require multiple authorization approvals before claims can be reimbursed.
Missing or expired authorizations are one of the leading causes of behavioral health claim denials.
Documentation requirements have also become more demanding. Payers now expect detailed clinical notes that clearly support medical necessity, treatment goals, patient progress, and session duration. Incomplete documentation can quickly trigger denials or payer audits.
Telehealth billing is another growing challenge. As telebehavioral health services continue expanding, providers must correctly manage telehealth modifiers, POS codes, payer-specific virtual care policies, and state licensing regulations.
Many behavioral health organizations are also dealing with staffing shortages, making it difficult to maintain consistent billing operations internally. As a result, practices often experience slow insurance follow-up, unresolved denials, and increasing accounts receivable.
The Hidden Revenue Leaks Affecting Behavioral Health Practices
Many behavioral health providers do not realize how much revenue they lose through inefficient revenue cycle management processes. Small operational issues can quietly create major financial losses over time.
For example, inaccurate eligibility verification may leave providers treating patients whose behavioral health coverage is inactive or limited. Incorrect behavioral health CPT coding can result in underpayments or denials. Delayed claim submission can trigger timely filing rejections, while poor denial follow-up often leaves recoverable revenue unpaid.
These problems directly impact practice profitability and cash flow.
At Velatrixa, we frequently help providers identify hidden revenue leaks that are preventing their practice from reaching full financial performance.
| Revenue Cycle Issue | Impact on Practice Revenue |
| Missed Authorizations | High-value claims denied |
| Eligibility Errors | Unpaid patient balances |
| Delayed Claim Submission | Timely filing denials |
| Poor Denial Follow-Up | Lost recoverable revenue |
| Incorrect CPT Coding | Underpayments and audits |
| Weak Documentation | Medical necessity denials |
Why Insurance Verification Is Critical in Behavioral Health Billing
Accurate insurance verification is one of the most important parts of behavioral health revenue cycle management. Before treatment begins, providers must confirm that behavioral health benefits are active and reimbursable.
This includes reviewing:
- Deductibles and copays
- Session limitations
- Referral requirements
- Behavioral health carve-outs
- Out-of-network coverage
- Prior authorization requirements
Many claim denials originate from incomplete eligibility checks completed during patient intake.
Behavioral health providers that fail to verify coverage properly often face unpaid claims, delayed reimbursements, and patient collection difficulties.
At Velatrixa, our insurance verification specialists conduct detailed benefit checks before services are rendered to help practices reduce denials and improve reimbursement accuracy.
Why Documentation Matters More Than Ever
Behavioral health reimbursement depends heavily on clinical documentation quality. Insurance companies now require providers to clearly document symptoms, diagnoses, treatment plans, patient progress, interventions, and session duration.
Generic or incomplete notes are one of the leading causes of behavioral health claim denials.
Behavioral health providers must also ensure that documentation supports the CPT codes billed on the claim. If payer auditors determine that documentation does not justify the billed service level, claims may be denied, downcoded, or flagged for audit review.
Strong documentation practices help providers improve claim approval rates while reducing compliance risks.
Common behavioral health CPT codes include:
| CPT Code | Description |
| 90791 | Psychiatric Diagnostic Evaluation |
| 90832 | 30-Minute Psychotherapy |
| 90834 | 45-Minute Psychotherapy |
| 90837 | 60-Minute Psychotherapy |
| 90853 | Group Therapy |
| 96130 | Psychological Testing Evaluation |
Claims Submission Is Only Half the Process
Submitting claims does not guarantee reimbursement. Successful behavioral health billing depends heavily on consistent claims monitoring, insurance follow-up, and denial management.
Behavioral health claims are commonly denied for authorization issues, telehealth billing errors, coding mistakes, eligibility problems, and medical necessity concerns.
Without a structured denial management process, practices often experience growing accounts receivable and major cash flow disruptions.
Many in-house billing teams lack the time and resources needed for aggressive follow-up and appeals management. As a result, denied claims remain unresolved for months or are written off entirely.
At Velatrixa, our behavioral health billing specialists actively track denied claims, identify payer trends, submit appeals, and recover delayed reimbursements before revenue is lost permanently.
| Common Denial Reason | Why It Happens |
| Authorization Denials | Expired or missing approvals |
| Medical Necessity Denials | Incomplete clinical notes |
| Eligibility Denials | Coverage not verified |
| Telehealth Rejections | Incorrect modifiers or POS |
| Timely Filing Denials | Claims submitted too late |
Why More Providers Are Outsourcing Behavioral Health Medical Billing Services
As reimbursement complexity continues increasing, many practices are outsourcing behavioral health medical billing services to specialized RCM companies.
Managing behavioral health billing internally requires experienced staff, continuous payer training, denial management expertise, and constant compliance monitoring. Maintaining an in-house billing department has become difficult and expensive for many providers.
Outsourcing behavioral health revenue cycle management allows practices to improve operational efficiency while reducing administrative burden.
Providers that outsource behavioral health billing services often experience:
- Faster reimbursements
- Lower denial rates
- Reduced administrative workload
- Improved cash flow
- Better accounts receivable management
- More accurate claims processing
Most importantly, outsourcing allows providers to focus more on patient care instead of dealing with insurance companies and billing backlogs.
| In-House Billing Challenges | How Velatrixa Helps |
| Staff burnout | Dedicated behavioral health billing team |
| Slow insurance follow-up | Aggressive AR management |
| Rising denial rates | Proactive denial prevention |
| Authorization backlogs | End-to-end auth management |
| Unstable cash flow | Faster reimbursements |
| Limited reporting visibility | Detailed financial reporting |
Why Behavioral Health Providers Choose Velatrixa
Velatrixa understands the unique reimbursement challenges behavioral health providers face every day. Our team specializes in behavioral health revenue cycle management and works closely with providers to improve financial performance through customized billing solutions.
We help mental health organizations strengthen every stage of the revenue cycle, including insurance verification, authorization management, behavioral health coding, claims submission, denial management, payment posting, AR follow-up, and revenue reporting.
Rather than offering generic medical billing support, we provide behavioral health billing services specifically designed for mental health and substance abuse treatment providers.
Our goal is simple: help providers reduce denials, improve collections, maximize reimbursements, and achieve long-term financial stability.
Final Thoughts
Behavioral health providers are under increasing pressure from rising denials, delayed reimbursements, and growing administrative workload. Without a strong behavioral health revenue cycle management strategy, these challenges can quickly turn into serious cash flow disruptions and financial instability.
A well-structured billing process can change that, reducing denials, improving collections, and bringing consistency and predictability to your revenue cycle.
At Velatrixa, we help behavioral health practices take control of their revenue cycle with specialized RCM services designed to reduce revenue leakage, speed up reimbursements, and improve overall financial performance.
Don’t let unpaid claims and billing delays keep draining your revenue. Partner with Velatrixa and strengthen your behavioral health billing before losses add up.
FAQs
Why is my behavioral health practice losing money even with full patient schedules?
Even fully booked practices lose revenue due to claim denials, missing authorizations, incorrect coding, and delayed billing follow-ups. In behavioral health, seeing patients does not guarantee payment unless the revenue cycle is managed properly.
What causes so many denied claims in behavioral health billing?
Most denials come from missing or expired prior authorizations, incomplete clinical documentation, eligibility issues, incorrect CPT coding, and telehealth billing errors. Without strong RCM processes, these small issues quickly turn into consistent revenue loss.
How do I know if my behavioral health billing process is broken?
Warning signs include rising accounts receivable (AR), frequent claim rejections, delayed insurance payments, staff constantly chasing denials, and unclear financial reporting. If cash flow feels unstable despite steady patient volume, your RCM needs improvement.
How can I reduce prior authorization issues in behavioral health billing?
The key is proactive authorization tracking, real-time verification, and continuous monitoring of payer requirements. Many practices lose revenue simply because authorizations expire unnoticed or are never updated during treatment.
Why are insurance companies denying behavioral health claims more often now?
Payers are applying stricter rules for medical necessity, therapy frequency, session duration, and documentation quality. Behavioral health claims are now reviewed more closely than ever, especially for long-term or high-frequency treatment plans.
Should I outsource behavioral health billing or keep it in-house?
Outsourcing is often more efficient for growing practices because it reduces staffing pressure, improves billing accuracy, and ensures faster denial resolution. In-house teams often struggle to keep up with payer changes and workload demands.
How can a medical billing company like Velatrixa improve my revenue cycle?
A specialized behavioral health billing partner like Velatrixa helps by improving claim accuracy, managing authorizations, reducing denials, following up on AR faster, and ensuring every step of the revenue cycle is optimized for maximum reimbursement.